 As an Infectious Diseases specialist seeing patients in the hospital, I treat patients on a daily basis for pneumonia. It is one of the commonest infectious diseases requiring patients seek medical attention.
As an Infectious Diseases specialist seeing patients in the hospital, I treat patients on a daily basis for pneumonia. It is one of the commonest infectious diseases requiring patients seek medical attention.
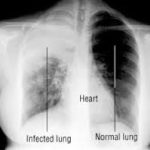
Simply speaking, pneumonia refers to an infection of the lungs. Any germ can infect the lungs, including bacteria, viruses, fungi, and even parasites. But by far the commonest causes are bacteria. Often, however, a bacterial pneumonia is preceded by a viral infection, typically of the upper respiratory tract. The virus may or may not spread to the lungs. Because the body is already weakened by the viral infection, it is easier for bacteria to take hold, spread to, and invade the tissues of the lungs, causing bacterial pneumonia.
In this post, I will address 7 questions that I am regularly asked by patients and their family members, and sometimes nurses, about pneumonia.
1 – How does one actually get pneumonia? Pneumonia may occur when germs which happen to be in the surrounding air, get inhaled into the lungs. It may also occur when bacteria normally present in the mouth and throat get breathed down (aspirated) into the lungs. Yet another (but very uncommon) way that pneumonia can occur, is if infection circulating in the blood stream lodges into the lung tissue.
Knowing how pneumonia can occur, it is clear that all of us are potentially at risk. Why then, don’t more of us come down with pneumonia? Because the immune system usually traps the germs, before they can invade the lungs. A dip in the strength of the immune system can cause pneumonia to develop. Also, if a person is exposed to a particularly high concentration of a germ, this can overwhelm the immune system and cause pneumonia to develop. Another reason for pneumonia to develop, is if the offending germ is particularly virulent (aggressive).
I often tell patients that pneumonia develops when all factors happen to align just perfectly at a particular point in time (dip in immune system + exposure to high load of virulent germ).
2 – Is pneumonia contagious? This is a common question, particularly from nurses. Especially nurses working on units with chronically ill patients on the ventilator, whose infections tend to be with bacteria that are resistant to many antibiotics.
Pneumonia from viruses is more contagious than that from bacteria. Viruses tend to cause more upper respiratory symptoms including sneezing. Sneezing causes respiratory droplets to be propelled further than with a cough, so theoretically more germs can reach other persons. Furthermore, because viral particles are much tinier than bacterial particles, respiratory droplets contain a much higher load of virus than bacteria. As noted before, the higher the concentration of germs that a person is exposed to, the greater the chance of coming down with infection.
Hospitalized patients with pneumonia tend to have bacterial rather than viral infection. Bacterial pneumonia is generally not contagious. We are not going to catch Streptococcus or Klebsiella pneumonia from another person. The patient would have to cough directly into a person’s face and then that person would have to at the same time, inhale the infectious droplets. Alternatively, if the environment in the patient’s room is heavily contaminated with their secretions, and someone touches a surface, then puts their contaminated fingers into their mouth or nostrils, they can possibly acquire the infection.
Very important, though, is the fact that the immune system will kill the bacteria in the upper airway, before they get a chance to progress into, and invade the lungs. Therefore the chance of “catching” pneumonia directly from another person, is generally small.
3 – How can a patient with pneumonia know when they no longer need supplemental oxygen? If pneumonia involves large sections of the lungs, it means that the primary function (transporting oxygen to the blood) is compromised. The patient therefore has to be given supplemental (extra) oxygen. Once the inflammation in the lungs starts improving and they are working better, less oxygen is required. The patient knows they are better when they are able to breath comfortably on normal room air without getting overly short of breath. Also, after mild exertion, if their oxygen level doesn’t fall below 90%, then supplementation is not required.
4 – Is it normal to have a hacking cough, even after several days of antibiotics? Even when a person with pneumonia is getting appropriate antibiotic coverage, it is not abnormal for them to continue to cough for days, and sometimes even weeks after completing treatment. Some inflammation of the lungs still remains after the infected lung tissue has be sterilized by antibiotics. Further, the cells lining the airways, that got damaged by the process of the infection, can’t all be gobbled up by the immune system. Those dead cells have to be coughed out with mucous.
5 – How soon after getting pneumonia can the flushot be taken? Theoretically, a person with pneumonia should get a flushot before leaving the hospital, once it’s influenza season, given that the opportunity to do so afterwards, may be lost. However, for a patient whose body is quite run down from a severe bout of pneumonia, the flu vaccine may not be as effective (baseline effectiveness is about 75%). The persons who get the best response are those with the strongest immune systems. So unless we are in the heart of flu season, my recommendation to the average patient is to wait about 2-4 weeks before getting the influenza vaccine. This gives extra time for the immune system and body to recover and so the chance of a more effective response is better. For a patient who is not expected to have a quick recovery, such as a nursing home patient, they are probably better off taking the flushot as soon as it is available, rather than wasting precious time.
6 – My mother got the “pneumonia vaccine” but still ended up with pneumonia. Why is that? This vaccine, the pneumococcal vaccine, protects against several strains of the bacteria Streptococcus pneumonia (pneumococcus). These bacteria are some of the commonest causes of pneumonia, but not the only cause. Additionally, there are some strains of pneumococcus that are not covered by the vaccine.
The pneumococcal vaccine may not significantly reduce the overall incidence of pneumonia, however it does decrease the chance of severe complications of pneumococcal infection such as meningitis and endocarditis.
The pneumococcal vaccine is indicated for adults over 65 years of age, and for persons with chronic medical conditions such as diabetes, heart disease, and chronic lung disease.
7 – How soon after recovery from pneumonia can one get back to regular activities? I usually tell patients to listen to their bodies. Don’t over exert yourself to the point where you feel as if you are going to faint. Take frequent breaks and you will notice improvement over weeks to months depending on how severe the pneumonia was to begin with.
 Lajune says
Lajune says
October 16, 2016 at 3:15 pmGood article
 infectiousmd says
infectiousmd says
October 17, 2016 at 11:34 amThank you! Please let us know if there is another topic you would like to see covered on the blog.