 I remember the first time I ever heard of shingles was as a young teenager when my great aunt told me she had it. She had gone to England to live for 3 years to help to take care of her grand children and got it while there. She would have been about 70 years old. The thing she spoke about the most when she got back home to the Caribbean is the severe pain she was still experiencing in the region on her hip where the shingles rash occurred. She never stopped believing that it was the cold in England that caused her to get shingles .
I remember the first time I ever heard of shingles was as a young teenager when my great aunt told me she had it. She had gone to England to live for 3 years to help to take care of her grand children and got it while there. She would have been about 70 years old. The thing she spoke about the most when she got back home to the Caribbean is the severe pain she was still experiencing in the region on her hip where the shingles rash occurred. She never stopped believing that it was the cold in England that caused her to get shingles .
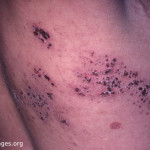
Shingles occurs when the chickenpox virus (called varicella-zoster virus) reactivates in the body. After someone recovers from chickenpox, the virus does not go away but remains dormant in the body in the roots of the nerves, kept in check by the body’s immune system (the police of the body that protect us from bad germs). Later on in life when the immune system gradually weakens, the virus can reactivate, causing shingles which is characterized by a rash and nerve pain (sharp, tingling) in the affected area. Because it is in the nerve root, reactivation would cause the rash to occur on the region of skin supplied by the infected nerve. That is why the rash occurs on one side (usually on the trunk but can be on the face or on one of the limbs), and does not cross the midline.
Shingles is most common in persons older than 60 years because of a gradual weakening of the immune system with age. Stressful situations such as a major surgical operation, a severe infection such as pneumonia, or a stroke can cause additional/sudden weakening of the immune system. That is why people tend to come down with shingles after such events.
For my aunt, I don’t think the cold temperature itself subjected her to shingles but instead, the stress of feeling cold all the time (having lived in the warm Caribbean her whole life!) combined with her being older, is probably what triggered her shingles. Seeing her discomfort, and that of my patients over the years, has made me hope that I never experience shingles myself.
Fortunately we now have a vaccine to prevent shingles, something that was not available to my aunt in the 80s and 90s. Now, the best vaccines (such as tetanus, hepatitis B, measles, etc) are more than 90-95% effective. The shingles vaccine, in comparison, prevents infection in only 51% of persons vaccinated. So half of everyone who gets the shingles vaccine will still end up getting shingles infection, which is a lot. Broken down by age group, the vaccine is most effective in the 60-69 year age group, preventing infection in 64% of cases, and least effective in the >80 year age group, preventing infection in only 18% of cases.
However, an additional benefit of the shingles vaccine, is that in persons who do get shingles after being vaccinated, the debilitating nerve pain that comes with it (post herpetic neuralgia) may be prevented. The nerve pain is prevented in 55% of persons 70-79 years old, and in 26% of persons >80 years old.
All in all, the shingles vaccine if not preventative in half of cases, decreases the severity of the rash and intensity of the nerve pain that comes with it.
The vaccine recommendations from the Advisory Committee on Immunization Practices (ACIP) are as follows:
– vaccination is recommended for all persons 60 years of age and older (it is FDA approved for ages 50-59 but not ACIP endorsed)
– it can be given to persons who have had shingles in the past; vaccinating 6-12 months after shingles may result in a better response to the vaccine
– no need to test for evidence of past chickenpox infection before giving the vaccine
– because the vaccine has live virus, it should not be given to persons with a severely weakened immune system such as someone undergoing chemotherapy, or with advanced HIV infection
Other recommendations regarding the shingles vaccine are:
– vaccination should be given to persons who are about to start treatments that will weaken the immune system such as cancer chemotherapy or rheumatoid arthritis drugs such as Enbrel. Timing of vaccination is suggested to be at least 4 weeks before starting such treatments
– in persons who will complete chemotherapy, wait 3-6 months after completing therapy before giving the shingles vaccine
– someone who never had chickenpox but got the chickenpox vaccine, has very low risk for shingles and therefore shingles vaccination is not recommended
The other day I had patient of about 75 years old who had a blistering rash on the abdomen. The patient did not even know about it as there was no pain and it was a doctor who saw it after lifting the examining gown. The rash involved a very small area next to the umbilicus on one side. Since it was so mild and painless, we tested to see if it was shingles or just a small patch of herpes. The test came back positive for the shingles virus. The patient had received the shingles vaccine about 5 years ago. This case is what made me appreciate more than ever, how much the shingles vaccine helps. This patient had absolutely no pain and only a mild rash and will likely not have prolonged, debilitating nerve pain.
I wholeheartedly agree with ACIP in their recommendation to vaccinate patients over 60 years of age against shingles. For those younger than 60 years old, the decision to vaccinate will be based on the individual’s particular situation. As always, seek advice from your personal physician for your particular situation.
One last thing…
You cannot catch shingles from someone since shingles is a reactivation of the chicken pox virus already in the body, and not a new infection. The only person at risk for getting infection from someone with shingles is someone who has never had chicken pox infection or the chicken pox vaccine. If this non-immune person comes into contact with fluid from a shingles blister, they can get the chicken pox infection (not shingles).
Leave a Reply